Endometriosis is a common gynaecological condition where the inner lining of the uterus (womb) grows in locations outside of the uterus. Endometriosis affects many women, and it has been estimated that up to 32% of women of reproductive age undergoing laparoscopy for investigation of pelvic pain will have some degree of endometriosis. Endometriosis is reported to affect over 176 million women worldwide. It is associated with female infertility, and is a common cause for painful sexual intercourse and painful periods.

Endometriosis may be more common in:

Endometriosis commonly affects the ovaries, and can be present as superficial implants on the surface of the ovaries, or as ovarian cysts known as “endometriomas”, which containing chocolate-coloured material. For this reason, endometriomas are often referred to as “chocolate cysts”.
Endometriosis can also often be found in other tissues within the pelvis, such as:
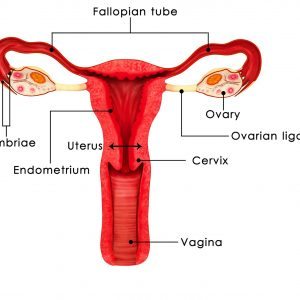
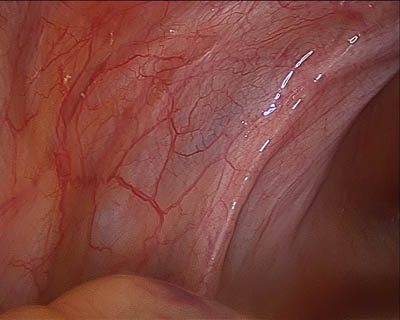
Endometriotic lesions can be obvious and extensive in nature, with involvement of important vital organs, such as the bowel or the ureters (which are the tubes draining urine from the kidneys to the bladder). Sometimes, endometriosis can be subtle, and can be easily missed by the untrained eyes. Importantly, studies have shown that even a small deposit of endometriosis can cause significant symptoms such as pain. Therefore, for the best chances of successfully relieving pain following endometriosis surgery, it is important that your gynaecological surgeon is able to recognise even subtle and more atypical endometriotic lesions, and that all of these endometriotic lesions are removed and treated completely.
Endometriosis may cause painful periods, sexual intercourse pain, or even pain on passing urine or faeces. Sometimes, endometriosis may present with more unusual symptoms, such as low back pain. Some women may have mild symptoms, whilst it may cause debilitating symptoms in other women. Some women with endometriosis are completely asymptomatic.
Endometriosis is also associated with reduced female fertility. This may be due to the endometriosis and adhesions causing distortion of the normal anatomy (e.g. kinking or obstructing the Fallopian tubes), but even in the absence of such structural abnormality, endometriotic lesions may release substances which are “toxic” to fertilisation and implantation of the pregnancy. Studies have found that surgical removal of endometriosis may help improve a woman’s chance of natural conception.
In order to make an accurate assessment of whether a particular woman may have endometriosis, a detailed history and clinical examination by your gynaecologist is important. Findings on physical examination may vary depending on the location of the endometriosis. Endometriotic lesions may be detectable as tender nodules within the pelvis.
A pelvic ultrasound scan may show endometriosis of the ovaries (“endometrioma”), however ultrasound scans cannot usually detect endometriosis in other parts of the pelvis.
Some women may require keyhole surgery (laparoscopy) in order to definitively establish the diagnosis of endometriosis. This also offers the opportunity to surgically remove and treat the endometriosis at the same time.
Endometriosis surgery is best performed by laparoscopy (key hole surgery). This allows the gynaecological surgeon the best view of the pelvis, enabling the surgeon to see all the pelvic tissues under magnification, and thus improving the surgeon’s ability to identify all of the endometriotic lesions, and to remove them all completely. Even small and subtle endometriotic lesions can cause severe pain, and therefore it is vitally important that the gynaecological surgeon carefully inspects all areas of the pelvis during the laparoscopy.
Endometriosis is staged according to the site and severity of involvement with the disease. There are several different systems for staging endometriosis. The most widely used staging system is the modified American Society of Reproductive Medicine staging system, which ranges from stage 1 (minimal endometriosis) to stage 4 (severe endometriosis). This staging system does not correlate with severity of the woman’s symptoms (e.g. a woman with stage 1 endometriosis can also have very severe pain).
Not all women with endometriosis requires surgery, and it is important to see your gynaecologist for an assessment of your particular situation. Whilst surgery is the only way to definitively confirm the diagnosis of endometriosis, empirical medical treatment for endometriosis may be tried even without a surgical diagnosis. Medications which may be useful in helping to relieve symptoms of endometriosis include:
Dr Ken Law is a gynaecological surgeon in Brisbane who specialises in the management of endometriosis and pelvic pain. He can offer treatment options for women in Brisbane with painful periods, intercourse pain, and chronic pelvic pain. For further information and to discuss your specific condition with a Brisbane endometriosis specialist, contact Dr Ken Law to arrange a consultation at Greenslopes Obstetrics and Gynaecology.
